Translate this page into:
Post-biopsy spontaneous air in vertebrae: A tell-tale sign of vertebral hemangioma

*Corresponding author: Dharmendra Kumar Singh, Department of Radiodiagnosis, Vardhman Mahavir Medical College and Safdarjung Hospital, New Delhi, India. dksinghrad@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Aggarwal A, Khanna G, Kumar N, Singh DK. Post-biopsy spontaneous air in vertebrae: A tell-tale sign of vertebral hemangioma. Indian J Musculoskelet Radiol. 2023;5:146-9. doi: 10.25259/IJMSR_35_2023
Abstract
Although most vertebral hemangiomas are asymptomatic and common incidental findings on radiographs and cross-sectional imaging, few atypical vertebral hemangiomas have aggressive imaging features and are clinically symptomatic. This atypical vertebral hemangioma poses a diagnostic dilemma and needs to be differentiated from aggressive vertebral neoplasm-like metastasis or plasmacytoma. Advances in radiological imaging, particularly MRI, help in differentiating atypical hemangioma from aggressive vertebral neoplasm to a certain extent; however, computed tomography-guided biopsy is often required for histopathological confirmation and further management. The aim of the case report is to highlight the finding of post-biopsy spontaneous gas bubble formation inside the vertebra in aggressive vertebral hemangioma, which helps to differentiate it from aggressive vertebral neoplasms.
Keywords
Vertebral hemangioma
Computed tomography-guided vertebral biopsy
Bone tumor
Aggressive hemangioma
Hemorrhagic vertebral metastasis
INTRODUCTION
Vertebral hemangioma is the most common primary tumor of the spine. Usually benign, this lesion is of vascular origin, and like hemangioma in other parts of the body usually involves a proliferation of normal capillary and venous structures. These lesions are usually an incidental finding on computed tomography (CT) and magnetic resonance imaging (MRI) of spine and frequently observed in radiographs of the thoracolumbar spine.[1-3] However, sometimes these hemangiomas present with atypical and aggressive imaging features such as the involvement of the whole vertebral body and/or posterior elements, and cortical expansion with associated soft-tissue lesions.[4,5] In such cases, this atypical vertebral hemangioma poses a diagnostic dilemma and needs to be differentiated from aggressive vertebral neoplasm-like metastasis or plasmacytoma. Advances in MRI, for example, apparent diffusion coefficient, chemical shift imaging, and T1W dynamic contrast enhancement kinetics help in differentiating atypical hemangioma from aggressive vertebral neoplasm; however, CT-guided biopsy is often required for histopathological confirmation.[6,7] Hemorrhagic sample in biopsy always poses a diagnostic difficulty to the pathologist. The appearance of a spontaneous gas bubble formation in the vertebra, immediately post-biopsy, is a suggestive feature of liquid-filled spaces of aggressive hemangioma rather than a solid hemorrhagic lesion. We, hereby, describe a post-biopsy tell-tale sign that can help us to detect aggressive hemangioma, distinguishing it from the neoplastic solid vertebral lesion.
CASE REPORT
A 60-year-old male patient presented to the department of orthopedics with complaints of back pain for 6 months. There were no neurological complaints, no comorbidity, or any history of drug intake or trauma. A physical examination of the patient revealed normal sensory and motor functions. The plain radiograph demonstrated the collapse of the T12 vertebral body. MRI of the thoracolumbar spine revealed low signal intensity on T1 and high signal on short-tau inversion recovery (STIR) in the posterior and anterior third of the vertebral body while the mid-third demonstrated low signal on both T1 and STIR sequence. The endplates and discs were relatively preserved. There was a posterior cortical bulge causing indentation on the spinal cord [Figure 1]. No obvious osteoporosis was appreciated in the radiograph and MRI of the thoracolumbar spine. There was no other vertebral lesion. Blood tests were normal. Based on the findings of MRI with no clinical history of trauma and the patient’s age, a suspicion of pathological vertebral collapse was suggested with differential diagnosis of solitary vertebral metastasis, plasmacytoma, and the remote possibility of atypical hemangioma.
For diagnostic workup and further management plan, CT-guided percutaneous biopsy of the T12 vertebral body was performed under aseptic precaution in a prone position by a superior costotransverse approach using a T-handle Jamshidi™ 11G (C.R. Bard, Inc.) needle. The biopsy sample obtained was hemorrhagic but, the appearance of spontaneous gas bubbles in the T12 vertebra, immediately after the biopsy was highly suggestive of atypical hemangioma rather than malignant neoplasm [Figure 2]. Hemangioma was later confirmed on histopathology [Figure 3].
DISCUSSION
Vertebral hemangioma is commonly encountered and is the most common primary tumor of the spine.[1] In an autopsy series, the incidence of vertebral hemangioma was found to be 11% in the adult population.[5] Histopathologically, it is the hamartomatous proliferation of endothelium-lined vascular tissue, which usually affects the skull and spine in the skeletal system. Most often, patients with vertebral hemangioma are asymptomatic, but rarely in 1% of cases, patients present with back pain and symptoms of neural compression.[8]
Most hemangiomas are diagnosed with radiological imaging. On radiographs and sagittal/coronal reformatted CT images, a typical jailhouse or corduroy appearance is seen due to prominent vertical trabeculae. On axial images, this is typically seen as a polka dot appearance. On MRI, the appearance of vertebral hemangioma depends on the fraction of lesion occupied by fatty stroma, vascular tissue, and the amount of interstitial edema. Typically, due to high-fat content, they appear as well-defined hyperintense lesions on both T1W as well as T2W sequences. Corresponding to the prominent vertical trabeculae, on the T1W sequence, few hypointense punctate areas can be seen. Due to serpentine vascular channels within the lesion, fluid-sensitive sequences such as STIR or fat-saturated T2 sequences, they appear slightly hyperintense. In the post-contrast MR imaging, variable enhancement is noted.
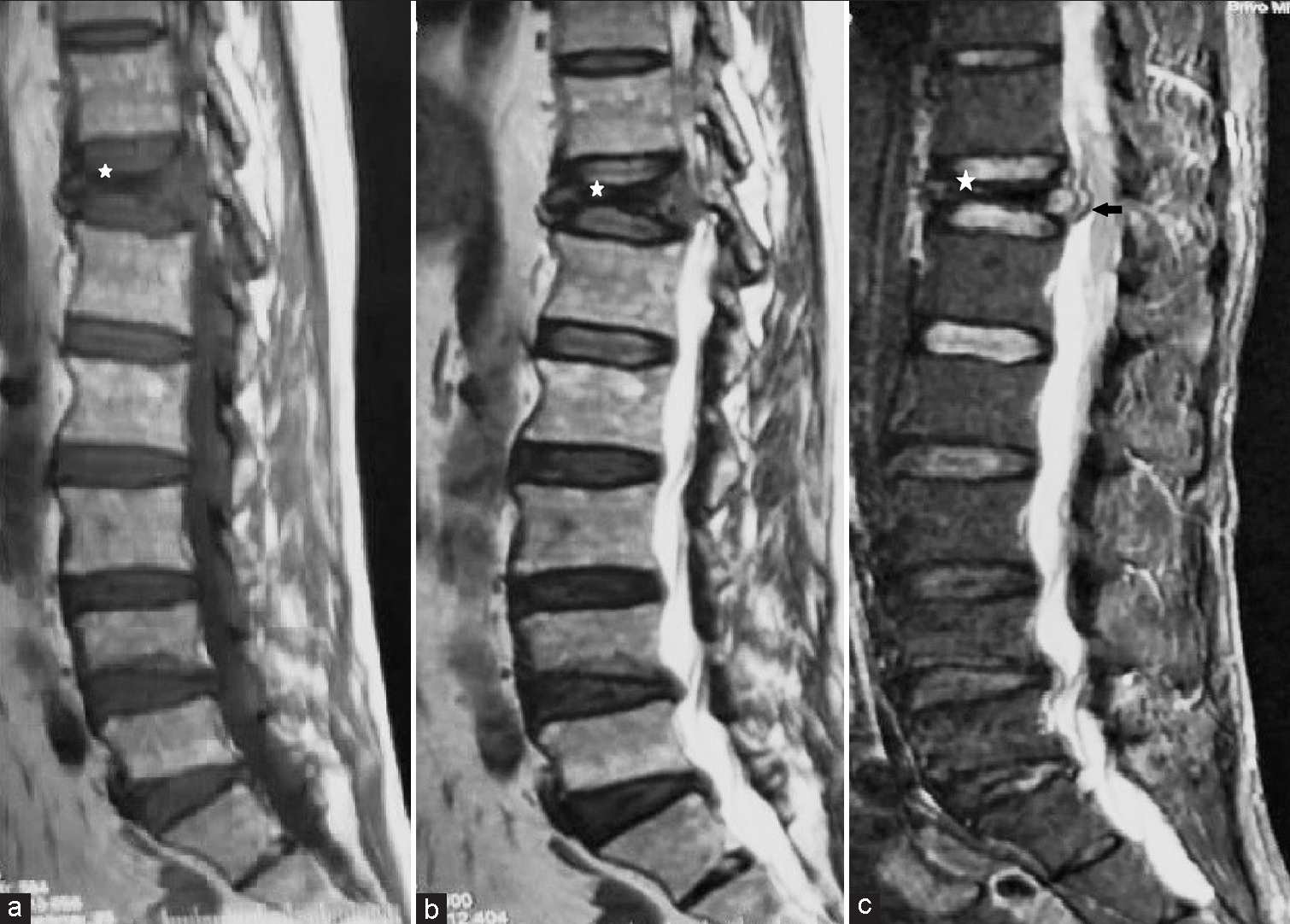
- (a) Sagittal T1, (b) T2, and (c) STIR MR images of the thoracolumbar spine demonstrate the collapse of the T12 vertebral body (white asterisk) with altered marrow signal. Posterior cortical bulge causing indentation of the spinal cord (black arrow) is demonstrated in figure 1c.

- (a) Axial, (b) sagittal, and (c) coronal reformatted computed tomography images of the T12 vertebra demonstrate gas bubbles in the vertebra (white arrow) after the biopsy of aggressive vertebral hemangioma (Black arrow-biopsy needle).

- Photograph demonstrates a lattice-like pattern of thin-walled blood vessels of various sizes with minimal atypia (Hematoxylin eosin coloration, magnification ×100) (black arrows).
Atypical hemangioma has a lesser fat content and more vascularity. Therefore, they show mixed (iso-to-hypointense) signal intensity on the T1W sequence and hyperintense signal intensity seen on the T2W sequence and STIR. On post-contrast MRI, a variable degree of enhancement is seen. Vertical trabeculae are more difficult to appreciate in atypical hemangioma.[4,5]
Few studies have shown encouraging results of T1W dynamic contrast-enhanced MRI in differentiating atypical hemangioma from vertebral metastasis based on the contrast-enhancement curves and quantitative analysis of KVp and Ktrans perfusion parameters.[6] The role of chemical shift imaging and diffusion-weighted MRI imaging has also been studied in differentiating atypical hemangioma with vertebral neoplasm.[7] However, histopathological confirmation of the lesion is still the gold standard for etiological confirmation.[8]
Unfortunately, the diagnostic yield of vertebral hemangioma biopsy is less due to the hemorrhagic sample, which may pose difficulty in differentiating it from aneurysmal bone cyst (ABC) and hemorrhagic metastasis.[9] In our case, the biopsy sample was hemorrhagic, but the spontaneous gas bubble appearance in the vertebral body after the biopsy was very suggestive of hemangioma. Later on, the histopathology also confirmed the same.
A possible explanation for the appearance of gas bubble phenomena in post-biopsy aggressive vertebral hemangioma is the presence of fluid-filled cavities connected by porous walls through which gas can diffuse. During vertebral biopsy, the negative pressure created in vertebrae allows nitrogen gas from vascular channels to diffuse through porous channels in the cavity. This is in contrast to any solid lesion such as plasmacytoma or hemorrhagic metastasis, which will not allow air to diffuse after the procedure. The primary ABC is a blood filled cavity lined by vascular endothelium with fibroosseous septations, rather than vascular channels, so during the biopsy of ABC, the spontaneous diffusion of air into the cavity is not observed. It is important to differentiate the iatrogenic push of air during vertebral biopsy versus post-biopsy spontaneous air in vertebral hemangioma. The post-biopsy spontaneous air in vertebral hemangioma is notably at a distance from the biopsy path as opposed to iatrogenic air push which is along or near to the biopsy path. The air distribution in post-biopsy hemangioma is arranged in a linear/tubular fashion along the trabeculae and spread over whole vertebrae, as opposed to iatrogenic push which is more of a bizarre pattern between the trabeculae and is localized.[10]
In a recent case report by Kim et al., they found similar findings in two histopathologically proven cases of vertebral hemangioma (gas web sign).[10]
This sign is practically essential due to two main reasons. Clinically, obtaining several biopsy samples from vertebral hemangioma can be potentially dangerous as it may lead to bleeding and compression of the spinal cord (particularly in the thoracic spine), and second, many times due to hemorrhagic content, the biopsy report may be false negative. Therefore, acquaintance with this sign can prevent the need for unnecessary repeated biopsies.[10]
The spontaneous formation of air bubbles is also seen in other conditions such as osteoporotic fracture (intravertebral vacuum phenomenon), and in acute exacerbation of degenerative disc disease (Knutsson’s phenomenon), vertebral osteonecrosis (Kummel disease), and vertebral osteomyelitis due to gas-forming bacteria. Thus, the presence of spontaneous airs in vertebrae favors a benign process. However, this new sign needs further studies with a larger sample size for assessing its true and exact diagnostic utility.
CONCLUSION
We encountered a case of aggressive vertebral hemangioma, the diagnosis of which was uncertain on clinicoradiological evaluation and was later confirmed on histopathology. Post-biopsy, the presence of gas bubbles in the vertebral body suggested its non-solid composition and benign nature. This sign can help in distinguishing aggressive hemangioma from hemorrhagic vertebral metastasis and solid vertebral tumors like plasmacytoma.
Ethical approval
The research/study complied with the Helsinki Declaration of 1964.
Declaration of patient consent
Patient’s consent is not required as patients identity is not disclosed or compromised.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The author(s) confirms that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Outcome of dorsolumbar vertebral hemangiomas presenting with neuraxial compression. Indian J Orthop. 2012;46:536-41.
- [CrossRef] [PubMed] [Google Scholar]
- Vertebral hemangiomas: Diagnosis, management, natural history and clinicopathological correlates in 86 patients. Surg Neurol. 1998;50:535-47.
- [CrossRef] [PubMed] [Google Scholar]
- Vertebral hemangiomas: Radiologic evaluation. Radiology. 1986;161:183-9.
- [CrossRef] [PubMed] [Google Scholar]
- A systematic approach to vertebral hemangioma. Skeletal Radiol. 2015;44:25-36.
- [CrossRef] [PubMed] [Google Scholar]
- Differentiating atypical hemangiomas and metastatic vertebral lesions: The role of T1-weighted dynamic contrast-enhanced MRI. AJNR Am J Neuroradiol. 2018;39:968-73.
- [CrossRef] [PubMed] [Google Scholar]
- Differential diagnosis of hemangiomas from spinal osteolytic metastases using 3.0 T MRI: Comparison of T1-weighted imaging, chemical-shift imaging, diffusion-weighted and contrast-enhanced imaging. Oncotarget. 2017;8:71095-104.
- [CrossRef] [PubMed] [Google Scholar]
- Lumbar vertebral haemangioma causing pathological fracture, epidural haemorrhage, and cord compression: A case report and review of literature. J Spinal Cord Med. 2011;34:335-9.
- [CrossRef] [PubMed] [Google Scholar]
- Accuracy of percutaneous CT-Guided spine biopsy and determinants of biopsy success. J Belg Soc Radiol. 2016;100:62.
- [CrossRef] [PubMed] [Google Scholar]
- Aggressive vertebral hemangioma: A post-bioptic finding, the gas web sign-report of two cases. BJR Case Rep. 2020;6:20190091.
- [CrossRef] [PubMed] [Google Scholar]






